Diabetic neuropathy is a condition caused by long-term high blood sugar levels that damage the nerves, most commonly in the legs and feet. While it may begin with mild symptoms such as tingling or numbness, the condition can gradually progress and affect the way a person moves. Many individuals tend to ignore these early signs, assuming they are a normal part of diabetes. However, diabetic neuropathy can significantly impact balance, walking ability and overall mobility if left unaddressed.
Movement is essential for independence and quality of life. When nerve signals are disrupted, the body struggles to respond effectively during daily activities. Understanding how diabetic neuropathy affects movement can help individuals seek timely care and prevent long-term complications.
Table of Contents
Loss of Sensation and Its Impact on Walking
One of the most common effects of diabetic neuropathy is reduced sensation in the feet. When nerves fail to send accurate signals, it becomes difficult to sense pressure, surface changes or foot position. This can make walking feel unstable and increase the risk of tripping or falling. People may notice that they shuffle their feet, walk more slowly or avoid uneven surfaces due to fear of losing balance.
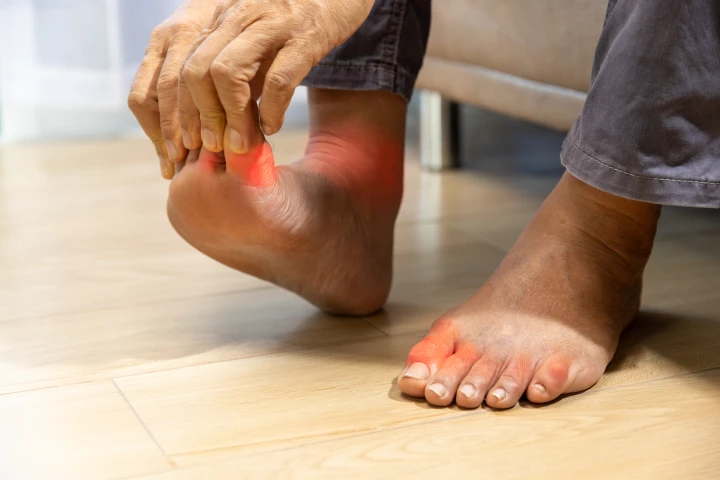
Over time, altered walking patterns can place extra strain on the ankles, knees, hips and lower back. These compensatory movements may lead to additional pain and joint stress, further affecting mobility and comfort.
Pain and Discomfort That Restrict Daily Movement
Pain caused by diabetic neuropathy can vary from mild aching to sharp, burning or electric-like sensations. This discomfort often worsens during activity or at night, affecting sleep and energy levels. To avoid pain, many individuals limit their movement without realising the long-term effects.
Reduced physical activity leads to muscle weakness, joint stiffness and decreased flexibility. As muscles become weaker, the body loses its ability to support proper movement, making everyday tasks such as standing, walking or climbing stairs more challenging. This gradual decline can significantly affect independence.
Balance and Coordination Challenges
Balance issues are another serious movement challenge associated with diabetic neuropathy. Nerve damage affects the communication between the brain and muscles, leading to poor coordination and delayed muscle response. Individuals may experience unsteady steps, difficulty changing direction or trouble maintaining posture.
Poor balance increases the risk of falls, which can be particularly dangerous for individuals with diabetes due to slower healing and higher risk of complications. Addressing balance issues early is essential for maintaining safety and confidence in movement.
Circulation and Its Role in Movement Health
Diabetic neuropathy is often associated with reduced blood flow to the lower limbs. Poor circulation can slow muscle recovery, increase stiffness and delay healing of minor injuries. Limited circulation also contributes to fatigue and discomfort during movement, making physical activity feel more difficult.
Physiotherapy treatment for diabetic neuropathy often includes techniques that support circulation, helping muscles and tissues function more effectively. Improved blood flow plays a key role in maintaining mobility and reducing discomfort.
How Physiotherapy Helps Manage Diabetic Neuropathy
Physiotherapy for diabetic neuropathy focuses on improving strength, balance, flexibility and movement control. A structured physiotherapy programme is designed based on individual needs and functional limitations. Treatment may include strengthening exercises, balance training, mobility exercises and education on safe movement practices.
Regular physiotherapy helps reduce pain, improve walking ability and restore confidence in daily activities. It also plays an important role in fall prevention and long-term mobility maintenance. Early physiotherapy intervention can slow the progression of movement limitations and support a better quality of life.
Supporting Long-Term Mobility and Independence
Managing diabetic neuropathy requires consistent care and attention to movement health. Along with medical management, physiotherapy treatment supports functional independence by addressing physical limitations before they worsen. Staying active under professional guidance helps individuals maintain strength, balance and confidence in movement.
Regaining Safer Movement through Physiotherapy for Diabetic Neuropathy
Movement challenges caused by diabetic neuropathy should not be ignored, even when symptoms appear mild. Early signs such as numbness, pain, stiffness or balance issues indicate the need for timely intervention. Physiotherapy treatment for diabetic neuropathy plays a vital role in improving mobility, reducing discomfort and supporting safer daily movement. At Sai Healthcare Foundation, personalised physiotherapy care is provided to help individuals manage diabetic neuropathy effectively and maintain long-term mobility through structured and supportive treatment approaches.